Easy Operation
– Easy to understand and operate.
– Device set up is quick and simple.
– Can be hung next to bed or placed next to patient on the bed.
– Little staff intervention required for monitoring and management..
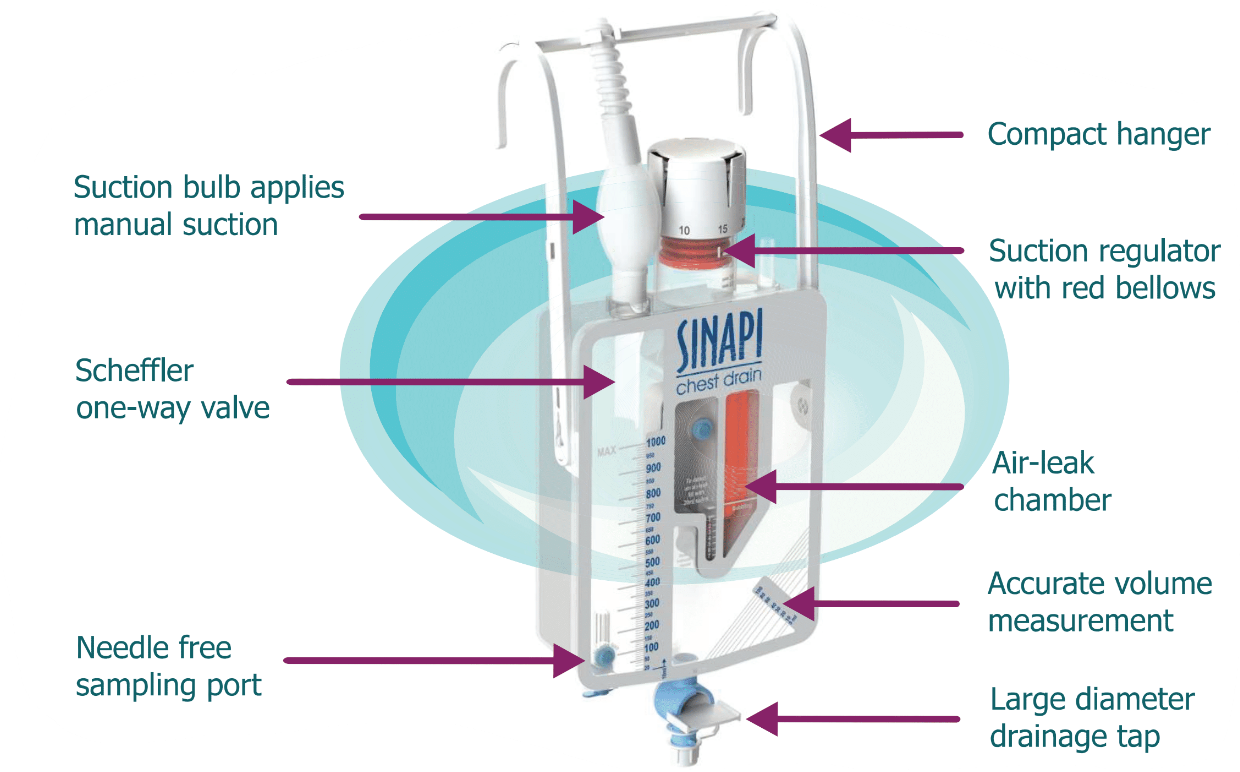
The SINAPI chest drain incorporates a mechanical (Scheffler) valve, allowing faster evacuation of liquids and air from the chest, makes patient management easier and supports early patient mobility.
Superior Patient Safety
– Simple design reduces risk of human error.
– Tube clamping never necessary.
– Can be oriented anyway without compromising closed system: safe to mobilise, reposition and transport patients.
– Suction regulator includes a high position pressure release valve and a high negativity vent.
– Red suction bellows provides visual confirmation that suction is applied.
– Fluid is drained into disposable bag, reducing risk of cross contamination.
Faster Drainage
– Valve is positioned before the collection chamber ensuring minimal dead space. Faster generation of negative intra-pleural pressure during breathing cycle and therefore earlier catheter removal.
– Valve has low opening pressure meaning low resistance to flow regardless of the volume of drained fluid. Results in faster drainage of air and fluid from the chest.
Early Patient Mobilisation
– The compact and lightweight design facilitates early mobilisation.
– Does not have to be kept upright at all times – can even be lifted higher than the patients.
– A shoulder sling provided to enhance patient comfort during mobilisation.
Clinical Evidence:
1. Shortens length of stay
1.1 Bertrandt, R.A., Saudek, D.M., Scott, J.P., Madrzak, M., Miranda, M.B., Ghanayem, N.S. & Woods, R.K. 2019. “Chest tube removal algorithm is associated with decreased chest tube duration in paediatric cardiac surgical patients.” Journal of Thoracic and Cardiovascular Surgery 1209–1217.
1.2 Cooper, C et al. 2006. “Xpand chest drain: assessing equivalence to current standard therapy– a randomised controlled trial.” SAJS 44 (4).
1.3 Takroni, M., Albarrati, A., Akomolafe, T. & al Enazy, M. 2021. The Effect of Early Mobilization on ICU and Hospital Length of Stay and Its Impact on the Cost of Care in Post-Open Heart Surgery Patients: A Randomized Control Trial (RCT). Journal of Heart Health.
2. Safer to use
2.1 Mattioli, S et al. 2008. “Survey on chest drainage systems adopted in Europe.” Interactive Cardio Vascular and Thoracic Surgery 7: 1155–1159.
3. Addresses OR/ICU Nursing shortage
3.1 Xu G, Zeng X, Wu X. 2021 Jul. “Global prevalence of turnover intention among intensive care nurses: A meta-analysis.” Nursing in Critical Care.
4. Regulated for outpatient management
4.1 Massongo, M., Leroy, S., Scherpereel, A., Vaniet, F., Dhalluin, X., Chahine, B., Sanfiorenzo, C., Genin, M., & Marquette, C.H. 2014. “Outpatient management of primary spontaneous pneumo-thorax: A prospective study.” European Respiratory Journal 43(2), 58.
4.2 Gogakos A, et al. 2015. “Heimlich valve and pneumothorax.” Ann Transl Med 3 (4): 54.
5. Less units used
5.1 Abdulsalam, Y. & Schneller, E. 2019. “Hospital Supply Expenses: An Important Ingredient in Health Services Research.” Medical Care Research and Review 240–252
